LARYNGEAL PAPILLOMA
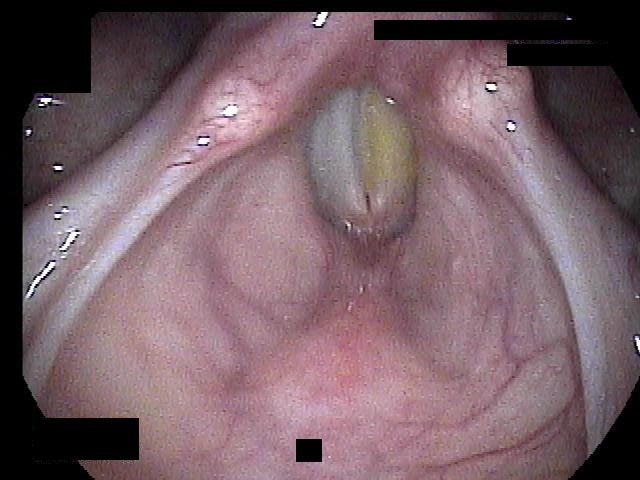
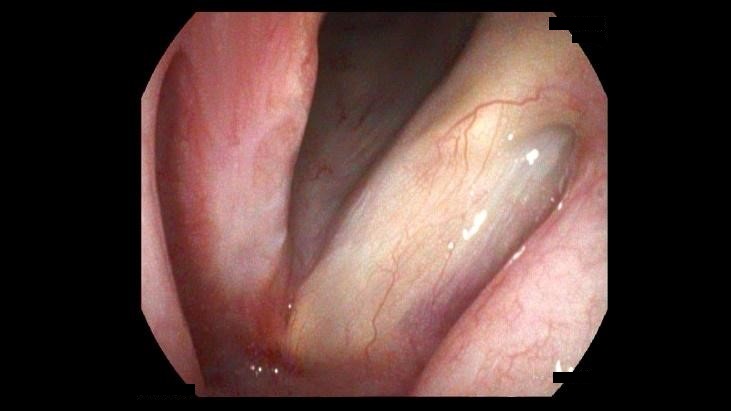
Laryngeal papilloma is caused by infection with human papillomavirus (HPV), particularly types 6 and 11. These growths can manifest as warty lesions and can occur in both children and adults, with the juvenile form often presenting more aggressively. Symptoms may include hoarseness, a raspy voice, difficulty breathing, and a sensation of a lump in the throat. Depending on their size and location, laryngeal papillomas can obstruct the airway and require treatment. Management often involves surgical removal, which may need to be repeated due to the tendency for recurrence. Regular monitoring is essential to manage symptoms and address any growth of the papillomas. While generally non-cancerous, the presence of these lesions necessitates ongoing evaluation, particularly in high-risk populations.













-1.jpg)
-2.jpg)




-1.jpg)
-2.jpg)